empowering the severely brain injured and their families via support, understanding and a network of care
Assessment and ICU
Once in the Accident and Emergency department, the initial hospital treatment following a brain injury will be an assessment by a doctor. The treatment of injuries will then be prioritised.
a doctor. The treatment of injuries will then be prioritised.
The patient may have been put into a Medically Induced Coma (MIC), this effectively shuts down the brain allowing time for it to recuperate, or they may have had a tracheotomy fitted. This is a surgical procedure in which an incision is made in the front of the neck and a breathing tube is placed into the trachea. This is needed if the patient is unable to breath normally.
As a relative this can be a confusing time and it may take some while before someone is able to speak to you.
- It is important that you stay calm.
- It is also helpful if you can have someone with you.
- Write down what the doctors tell you, ask that you be kept informed with the treatment and what the following stages are likely to be.
Assessing the Brain Injury
There are several imaging techniques that can help diagnose and assess the extent of the brain injury. The following scans are generally used and most effective.
- Computed Tomography (CT) scan.
- Magnetic Resonance Imaging (MRI)
- Functional Magnetic Resonance Imaging (FMRI)
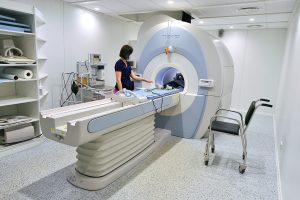
CT scans provide greater detail than a standard X-ray and can see blood vessels, nerves, tissues and other structures in and around the brain. It can therefore show brain bleeds, fractures of the skull and fluid build up which will lead to increased cranial pressure.
MRI scans are able to detect smaller injuries and detect damage within the brain. It uses magnetic fields and radio waves to take pictures of the inside of the body. This helps doctors and other medical staff see normal and abnormal areas of the brain. An MRI scan can show how and where blood is flowing in the brain.
FMRI scans are a special type of MRI. This scan helps doctors evaluate the blood flow due to chemical changes in the blood. It shows which parts of the brain are activated when asked to perform certain tasks, such as movement, memory and language.
Treatment of the Brain Injury
Following the scan the doctors will decide what initial treatment is required. If they have seen a blood clot, pooling of blood or a build up of cerebral fluid (oedema) an operation will be needed. However, it may be the case that the patient is left in an induced coma to allow the brain to rest.
If an operation is required a flap of bone is cut out of the skull, a Craniotomy Flap, which will allow the clot, blood or fluid to be removed. The bone will then be replaced, however in certain circumstances the bone may be left out and replaced later on in the recovery process. This decision is usually made during surgery.
Whether an operation is necessary or not the patient will be transferred to Intensive Care (ICU).
Intensive Care (ICU)
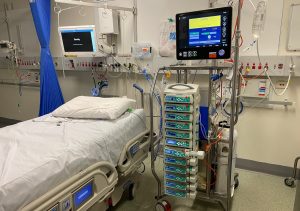 Patients on ICU will be looked after closely by a team of highly trained staff, 24 hours a day. There will normally be 1 nurse for every 1 or 2 patients and will be connected to specialised equipment by tubes, wires and cables. This equipment is used to monitor their health and support their bodily functions.
Patients on ICU will be looked after closely by a team of highly trained staff, 24 hours a day. There will normally be 1 nurse for every 1 or 2 patients and will be connected to specialised equipment by tubes, wires and cables. This equipment is used to monitor their health and support their bodily functions.
Equipment that may be used on an ICU includes:
- Ventilator is a machine that helps with breathing. A tube is placed in the mouth, nose or through a small cut in the throat (tracheostomy). This is to maintain the correct levels of oxygen whilst the brain continues to rest.
- Monitoring equipment is used to measure important bodily functions, such as heart rate, blood pressure and the level of oxygen in the blood. As the brain has been injured it is important that these functions are maintained at normal levels, if not relevant drugs can be administered.
- Intravenous lines and pumps. Tubes will be inserted into a vein (intravenously) to provide fluids, nutrition and medication.
- Feeding tubes are placed in the nose, or through a small cut made in the tummy or into a vein if a person is unable to eat normally.
- Drains and catheters are used to remove any build-up of blood or fluid from the body. Catheters are thin tubes inserted into the bladder to drain urine.
In addition to the above, the nurses will also be assessing the patient using other methods. This includes the Glasgow Coma Scale (GCS). This scale assesses patients according to three aspects of responsiveness: eye opening, motor, and verbal responses. Severe brain injuries score 3-8, moderate brain injuries score 9-13 and mild score 14-15.
From 2019 an updated system, known as the GCS-pupils system was published. This system aims to assist with assessing the prognosis of a brain injury.
What you and your loved one might experience in ICU
The aim of the medical team is to keep the patient stable using the equipment already mentioned. However, this treatment will need to be reduced over time allowing the doctors to see the patients response and their ability to cope on their own.
Neurostorming
Our brain allows us the have a ‘fight or flight’ response which responds to dangerous or high stress situations. When activated the vital functions, such as heart rate, blood pressure and body temperature regulation increase. After a severe brain injury this may stop functioning properly as the brain cannot determine if the body is still in danger. This is called Neurostorming or just Storming and it can happen at any time. Storming can be unprovoked or brought on whilst being given personal care, repositioned in bed, changes in mediation, sudden noises or other stimulation.
As the patient is in a coma or similar state of unconsciousness they will be unaware that this is happening. However, what they will be experiencing and what you may see are the following:
- profuse sweating (large globules of sweat)
- rigid arms and legs, downward pointed toes, arched spine and neck
- tachycardia – heart rate over 130 beats per minute
- hyper tension – high blood pressure
- high temperature – over 38.5c
- tachypnoea – rapid breathing, over 40 breaths per minute
Most treatments for Neurostorming involve mediations which focus on slowing the body’s stress response or relaxing the body.
Muscle weakness or Spasticity
Due to the injury, the brain doesn’t send the correct messages to the muscles. This can result in muscle weakness or muscle contractures, called spasticity. It is often rapid, occurring as early as one week following the brain injury.
This will require treatment and therefore you may well see limbs being splinted to maintain the range of movement.
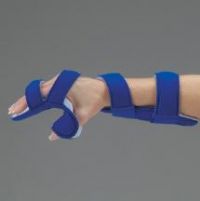
This picture shows a hand splint which helps stop reflexive contractures.
Contractures are the shortening and hardening of muscles, tendons or other tissue, which often leads to deformity and rigidity of joints. 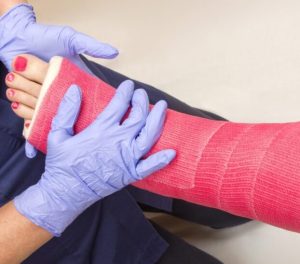
This is a foot cast which helps the foot from dropping.
Foot drop can occur when there is a disruption in communication between the nervous system and the muscles that lift the foot as a result of the brain injury.
What you can do to help your loved one whilst visiting in ICU
As the brain will need a lot of ‘rest time’, visiting is usually restricted. This is precious but also important time that you will have with your loved one. As they cannot always respond it can feel difficult or strange as the interaction will be one way.
You can tell them about your day, family life at home or things of interest to them.
You can bring in a book or newspaper to read to them.
Play their favourite music to them.
If their eyes are open show familiar photos to them.
Touch can also help.
Wear a recognisable perfume/after shave.
With any of the above or other ideas you may have, always ensure you check with the staff as some things can cause over stimulation.
What happens next?
Once your loved one is out of the ’emergency stage’ and there is less need for intensive nursing they may be moved into a General Hospital Ward or High Dependency Unit. They will most likely be still highly dependant of nursing care and need such things as hoisting, personal care and tube feeding. You may feel as if you want to become more involved with the care being given and this can be discussed with the nurse in charge.
This period of time can be very stressful for the family members as the ‘one to one’ care is no longer there. The nursing staff do their utmost within the ward but have a number of patients to look after. It is therefore so important, particularly if your loved one cannot communicate, that you become their voice, and ensure that you are kept fully informed of ongoing treatment and care. Don’t be afraid to keep asking questions and if you want to be with your loved one outside visiting hours check with senior staff.
There will be an ongoing assessment from the hospital team where it will be determined as to what the next stage will be. This could be to a rehabilitation unit, a care home or a discharge back home.